Youtube kanalımız ile çalışmalarımızı canlı olarak görün!
"İçeriklerimizden haberdar olmak için abone ol butonuna tıklamayı unutma! Abone olarak topluluğumuza katılabilir ve en yeni içeriklerimizi ilk sen izleyebilirsin."
Uygulanan İşlemler
Sıkça Sorulan Sorular
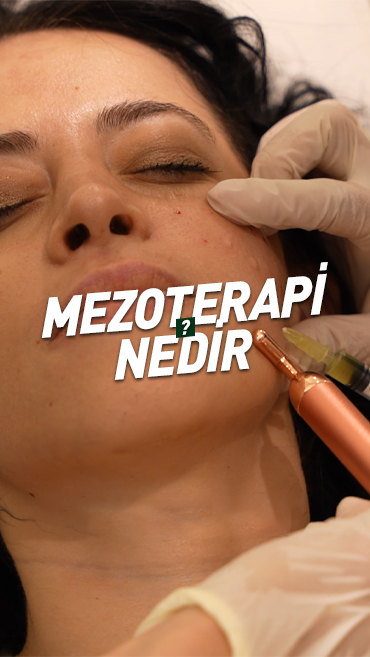
Doktorumuzla görüştükten sonra kliniğimizde bulunan fotona lazer cihazımız ile birlikte uyguladığımız mezoterapi ürünleriyle ameliyatsız yanak ve gıdı eritmek mümkündür. Günlük aktiviteleri etkilemeyen bu iki işlemde de hafif kızarıklık ve ödem harici bir etki görülmemektedir. Seans aralıkları ve sayısı kişiye göre değişkenlik göstermektedir.
Ameliyat sonrası oluşan morluklar genellikle 1 hafta 10 gün içerisinde iyileşmekte olup, kişinin yapısına göre değişkenlik gösterebilmektedir.
Ameliyatta süt bezlerine ya da süt kanallarına dokunulmamaktadır, bu nedenle emzirmede herhangi bir problem beklenmez.
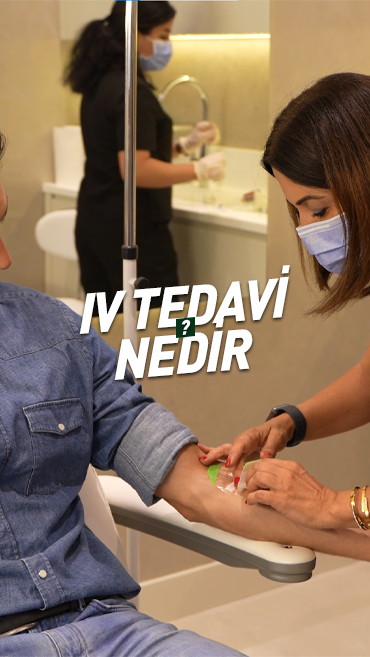
IV antioksidan ve vitamin tedavisi hekim ile görüşülüp, muayeneniz yapıldıktan sonra belirlenen ihtiyaca göre yapılır.
IV tedavi uygulamasında bir kateter veya iğne yoluyla damar sistemine vitamin ve antioksidanlar serum içine katılarak ya da doğrudan enjekte edilir.
Yüz bölgesinde uygulanacak olan iple askılamanın etkileri hastadan hastaya farklılık göstermektedir. Ancak genel itibarıyla 18 ay ile 24 ay arasında süren bir etkiden bahsetmek mümkündür. Etkinin uzaması adına hekiminizin önerilerini dikkate almalısınız.
Hayır. Botoks yapıldıktan sonra etkisi 3 günden itibaren başlar. 7-10 gün etkisi artarak devam eder.
- Bağışıklık sistemini güçlendirir
- Kan dolaşım sistemini, lenf sistemini, karaciğer ve böbrekleri temizler.
- Metabolizmayı destekler ve hızlandırır.
- Hastalıkların önlenmesi ve tedavisinde etkilidir.
- Hormonal dengenin sağlanmasında etkilidir.
- Yaşlanmayı geciktirir.
- Vücudun yenilenmesini ve canlanmasını sağlar.
- Ruhsal ve fiziksel bütünlük ve dengeleme sağlar.
- Zararlı bakteri, virüs, parazit, maya, küfü yok eder.
Hemen sonrasında duş alabilirsiniz.
1 ay sonra hafif spor, 2. Aydan itibaren tempoyu arttırarak spor yapabilirsiniz.
1.aydan sonra cinsel hayatınıza geri dönebilirsiniz.

Videolar